Without Agrippon
Email threads, spreadsheets, phone calls
Agrippon is the HIPAA-compliant task management tool built for billing teams. It centralizes communication, clarifies ownership of tasks, and gives teams a clear system for managing claims so work moves forward instead of stalling.
Designed to bring simple, structured communication to
dental practices, DSOs, and medical billing companies.
Many dental billing teams operate in environments where staffing is tight, roles overlap, and everyone is juggling multiple responsibilities.
When insurance follow-ups rely on scattered tools, teams spend valuable time searching for information that should already be visible.

When teams operate this way, follow-ups stall, communication breaks down, and claims age simply because no one has a clean line of sight.
Agrippon provides a structured workspace where dental offices
and billing teams manage claim follow-ups together.
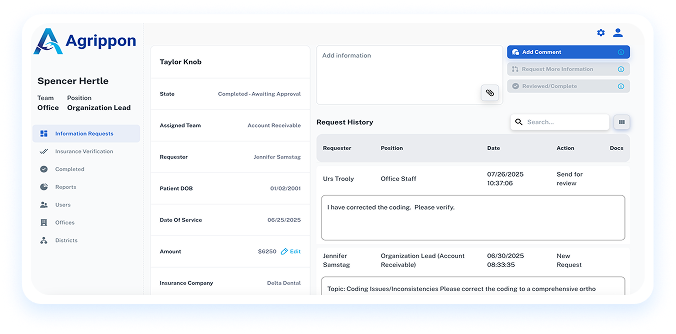
Agrippon provides a structured workspace where dental offices
and billing teams manage claim follow-ups together.
Most billing teams spend time managing the chaos around claims rather than actually resolving them. Agrippon removes the operational gaps that create unnecessary work.
Email threads, spreadsheets, phone calls

Structured workflow timeline with clear ownership
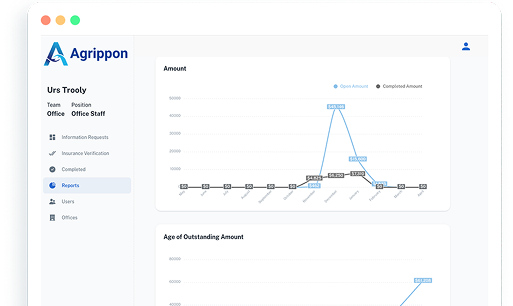
Most claim delays are not clinical issues. They are administrative
breakdowns in communication, documentation, and follow-up.
For a pThe Agrippon Guided Launchractice submitting 1,000 claims per month with an average value of $150, even a small number of preventable delays can represent more than $9,000 in monthly revenue at risk.
The revenue already exists. What many organizations lack is a workflow system that consistently moves claims toward resolution.
Agrippon provides the structure to do that.
Days 1-30
We offer a launch introduction covering functionality, key workflows, coaching tools, and analytics so teams understand how the platform supports their daily work.
Day 30
Leaders receive a review showing product adoption across offices or teams, highlighting which features are being used and where additional coaching may help.
Days 31-60
We collaborate with leadership to review workflow performance, reporting insights, and opportunities to improve adoption.
Days 61-90
A final review ensures teams are fully operational and provides recommendations for sustaining adoption moving forward.
The guided launch helps leadership build accountability and ensures the platform becomes part of the team's daily workflow rather than another tool that gets abandoned.
Different organizations require different levels of rollout guidance depending on size,
leadership availability, and geographic structure.
Tier 1
Launch presentation and product orientation.
Tier 2
Launch presentation plus 30-day adoption review, 60-day coaching collaboration, and final 90-day adoption review.
Tier 3
Weekly support in month one, bi-weekly collaboration in month two, adoption coaching, and structured client-led presentations.
Many billing teams start with the same operational challenges: scattered communication, missing documentation, and claims aging due to broken workflows.
dental insurance claim delays reduced by 50%
uncovered over $120,000 in aging claims
improved transparency and trust between offices and billing teams
When follow-up workflows become visible and structured, claims move faster and teams regain confidence in their billing process.
Agrippon supports organizations responsible for managing insurance follow-ups and maintaining revenue performance.
 Revenue cycle leaders
Revenue cycle leaders Billing managers
Billing managers Office managers
Office managers DSO operations leaders
DSO operations leaders Third-party billing organizations
Third-party billing organizationsAdding structure will.